In May 2019, The Atlantic published an article called The Truth About Dentistry.
It followed an unfortunate tale of Dr John Roger Lund, a dentist who subjected many of his patients to reckless overtreatment.
Some shocking anecdotes come out of this story, such as one of Dr Lund’s patients having nine root canals, and although such poor practice indeed deserve calling out, the article takes the further step in claiming that the whole dental profession is skewed towards the overtreatment of patients.
The article points to three main factors that facilitate a type of “cowboy dentistry”:
- That the imbalance of power between dentists and patients means that patients feel that they have no choice but to agree to suggested treatments.
- There is a lack of self-scrutiny and evidence based practice in dentistry, meaning that treatments are not as effective, or free of risk as some dentists make out.
- The costs of dental school and running a practice make overtreatment necessary in order to make a living. The fact that so many dentists operate in independent practices allows this overtreatment to go unchecked.
To evaluate how fair each of these points are we should go through each of them in turn.
Do dentists have too much power over their patients?
The author claims that, on the whole, patients do not feel like they can question their dentist about the suitability of suggested treatments.
This level of compliance is contrasted to interactions with other medical professionals such as cardiologists:
“In other medical contexts, such as a visit to a general practitioner or a cardiologist, we are fairly accustomed to seeking a second opinion before agreeing to surgery or an expensive regimen of pills with harsh side effects. But in the dentist’s office—perhaps because we both dread dental procedures and belittle their medical significance—the impulse is to comply without much consideration, to get the whole thing over with as quickly as possible.”
So the author claims that the causes of this asymmetry between people’s interactions with dentists and other medical professionals are a hatred of dental visits, and a playing down of the significance of dental treatments to one’s wider health and well being.
Well, what can be done to alleviate these problems?
As far as the unpleasantness of dental appointments goes, this is indeed a well established phenomenon—as indicated by the survey cited by the author that suggests that 61% of people are apprehensive about seeing the dentist.
What exactly is it about dental appointment that makes them so much more fear inducing than seeing any other kind of medical specialist?
I’d argue that a large part of it is down the body language forced onto a patient during a visit to the dentist.
Laying back in the dentists chair with your mouth open is an incredibly submissive position, and is one that is rarely repeated in any other situation.
Add to that the invasiveness of having your mouth prodded and inspected, and you can understand why such an experience may cause the “mental limpness” (author’s words) that may lead to an unusual level of compliance with any suggested treatments from the dentist.
To readdress this imbalance of power, perhaps there should be a short (few days, perhaps) “cooling off” period between examination and suggestion of treatment in order to allow any “mental limpness” to dissipate.
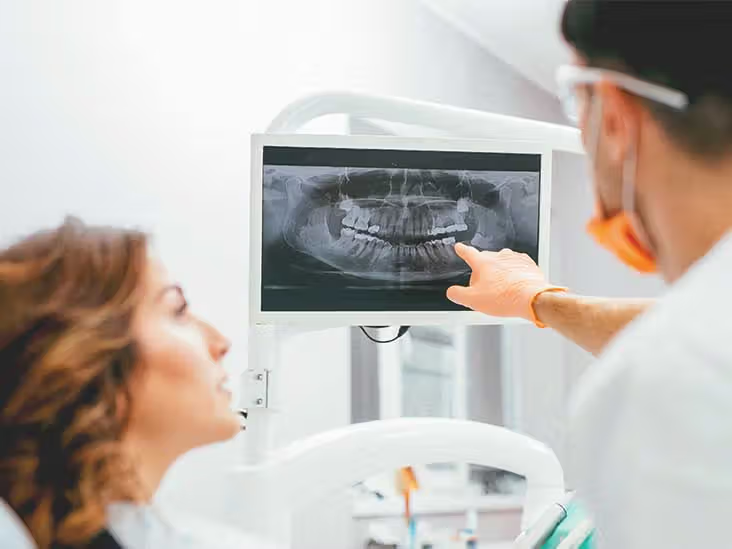
When it comes to the recommendation of treatments, a dentist should be as transparent as possible.
Patients should be able to see the x-rays and photos used to inform their dentist’s choice of treatment, and dentists should lay out all of the treatment options available as well as their various consequences (both financial and physiological).

That being said, effective patient communication and bedside manner is not taught in any structured way through dental school, and is certainly not a requirement for getting the qualifications needed to practice as a dentist.
Perhaps this is a point of improvement for the whole dental profession.
As for people’s downplaying of the significance to their overall health of dental treatments, I can only speak from my own experiences but I have not found this to be the case.
While it is in part up to the dentist to educate their patients about the wider medical implications of any dental issues and their treatment, wider public health education and society more generally also has a role to play in bringing dental education up to speed with education in other areas of medicine.
Is dentistry less evidence based than other medical fields?
The evidence for the author’s claims that dentistry is less grounded in evidence than other areas of medicine is shaky to say the least.
Dentists practice according to guidelines set out by The National Institute of Health and Care Excellence (NICE). This puts dentists on an equal footing with all other medical practitioners.
Dental procedures are informed by the Cochrane Institute who advise on evidence based dentistry, this again holds equally true for dentists as it does for other medical professionals.
The author claims that most of the Cochrane Institute’s reviews fail to confirm the benefits of dental interventions, either due to a lack of conclusive evidence, or to a lack of evidence more generally.
I’d argue that the use of the very phrase “lack of conclusive evidence” demonstrates a fundamental misunderstanding of the scientific method on the behalf of the author.
Progress in medicine (and both dentistry and general medicine fall into this bracket) is all about refinement.
Best practices are born out, but are constantly being tested, slowly changed and improved upon.
Both medical and dental best practices are vastly different to 20 years ago, and will be even more different in 20 years time.
The day that we conclude that a certain treatment is “the answer” to a specific problem is the day that we move away from a truly evidence based approach.
The author tries to ground his arguments for the lack of an evidence based approach in dentistry through examples of supposedly misinformed dental “truths”, some of which he has clearly misunderstood himself.
One such example is his criticism of the recommendation of daily flossing:
“Some data suggest that regular flossing, in addition to brushing, mitigates gum disease, but there is only ‘weak, very unreliable’ evidence that it combats plaque.”
Flossing is recommended to help prevent gum disease. Brushing removes plaque from teeth.
If indeed, there is only weak evidence that flossing removes plaque then that is neither here nor there. Its akin to saying that Vitamin C should not be recommended for general health reasons because it does not lower blood pressure. That simply isn’t its function
The author is, however, correct when saying that certain invasive procedures are becoming seen as less necessary:
“Little medical evidence justifies the substitution of tooth-colored resins for typical metal amalgams to fill cavities.”
And:
“As for common but invasive dental procedures, an increasing number of dentists question the tradition of prophylactic wisdom-teeth removal; often, the safer choice is to monitor unproblematic teeth for any worrying developments.”
This is all true, however the author does not appreciate that the dental profession is aware of this, and that “minimally invasive dentistry” is one of the biggest trends in the profession at the moment.
The author’s other piece of evidence for the lack of evidence-based-practice in dentistry is a field experiment demonstrating the amount of variation in dentists’ recommended treatment for the same case:
“A team of researchers at ETH Zurich, a Swiss university, asked a volunteer patient with three tiny, shallow cavities to visit 180 randomly selected dentists in Zurich. The Swiss Dental Guidelines state that such minor cavities do not require fillings; rather, the dentist should monitor the decay and encourage the patient to brush regularly, which can reverse the damage. Despite this, 50 of the 180 dentists suggested unnecessary treatment.”
This study, or at least the way that its results are presented by the author, greatly oversimplifies how dental problems are diagnosed and treated.
It is not simply the state of someone’s tooth, in isolation, that determines the best treatment for a patient.
Rather other factors such as their sugar intake, oral hygiene habits, and history of tooth decay plays a role.
Now admittedly this study concerns the rate of clinical variation over one case, so all of these factors would have been the same, however the complexity of oral health “in the real world” means that blanket guidelines will never provide the answer in every situation.
This phenomenon can also partially explain why clinical variation exists across all fields of medicine.
In a wider study measuring variance in treatments for a range of general medical problems, researchers for CareTrack found that “appropriate” care (according to national guidelines) was only administered in 57% of cases.
Health is a complex matter, so clinical variation is inevitable. The rate of such variance highlighted in these studies is problematic (don’t get me wrong here), but clearly the problem exists across the whole spectrum of medicine.
In short, I’m not sure if the author’s arguments for a lack of an evidential base to dentistry hold up.
Are dentists enabled and incentivised to recklessly over treat patients?
The final argument laid out in this article is that financial pressure and a lack of high-level regulation motivates and enables dentists to over treat their patients.
Let’s look at the author’s claims of a lack of regulation first.
The author writes:
“When physicians complete their residency, they typically work for a hospital, university, or large health-care organization with substantial oversight, strict ethical codes, and standardized treatment regimens. By contrast, about 80% of the nation’s 200,000 active dentists have individual practices, and although they are bound by a code of ethics, they typically don’t have the same level of oversight.”
While its true that dentists tend to operate in smaller practices than other medical professionals, a new dentist still has to work under supervision for the first two years of their career (in the UK at least).
The author argues that working for a large organisation implies that an individual practitioner’s decisions will be subject to a greater level of scrutiny, but is this actually true?
Given how overstretched some of the largest hospitals (in the UK at least) are, I would say that the answer to this is probably no.
This, answer is again backed up by studies into variance in clinical decision-making. What few studies there are do not suggest that such variance is higher in dentistry than in other medical fields.
When claiming that financial pressure incentivises overtreatment, the author writes:
“In parallel with the rising cost of dental school, the amount of tooth decay in many countries’ populations has declined dramatically over the past four decades, mostly thanks to the introduction of mass-produced fluoridated toothpaste in the 1950s and ’60s. In the 1980s, with fewer genuine problems to treat, some practitioners turned to the newly flourishing industry of cosmetic dentistry, promoting elective procedures such as bleaching, teeth filing and straightening, gum lifts, and veneers. It’s easy to see how dentists, hoping to buoy their income, would be tempted to recommend frequent exams and proactive treatments—a small filling here, a new crown there—even when waiting and watching would be better. It’s equally easy to imagine how that behaviour might escalate.”
The point about cosmetic dentistry is a fair one.
This field is both incredibly lucrative, and is rapidly growing due to the current fashion of having large, whiter than white teeth.
This look can only be achieved with veneers, often in conjunction with other cosmetic treatments like orthodontics.
So yes, for a dentist who is focussed on making a lot of money, cosmetic dentistry is the route to go down.
Is this problematic for the overall state of oral health?
Possibly yes.
Certain cosmetic treatments, such as veneers, can compromise your oral health in the long term.
We see the same problem when it comes to medical treatments administered purely for cosmetic purposes.
A balance between what a patient wants, and what can be done without harming their health in the long term needs to be found. It is the medical or dental professional’s job to do this and it is not always easy.
As for the temptation to recommend unnecessary examinations and treatments, while this may be true for dentists who do not have an established patient base, in general dentists who refrain from administering unnecessary treatments have happier patients.
Therefore, even though less money is made per patient, their patient base should grow faster as a reputation is developed for not bleeding patients dry.
Such long-term thinking probably wont appeal to all, and I’m sure that for dentists where their patient base is thin, or who practice in a remote location where there is a ceiling for how many patients they can actually have, the temptation to over-treat may be very real.
Dentists are in a position of great power and should have the responsibility to have their patient’s best interests at heart. However, they do benefit financially from more complex treatments and this does leave the door open to conflicts of interest, either due to of greed or desperation.
And while there is some regulation and accountability when it comes to clinical decision-making, monitoring every single dental appointment is not feasible.
Responsibility for the correct administration of oral health treatments should therefore come, in part, from the patient.
The reasoning behind a recommended treatment should be questioned, second opinions should be solicited, and improper conduct should be reported.
If fear and a lack of knowledge prevent this from happening, then it is up to dentists, public health educators, and attitudes towards dentistry more generally to address this problem. The bridge needs to be built from all sides.
If the author’s intention was to make readers more aware that dentists are fallible, and that prevention is preferable to procedure in dentistry then his cause is noble.
Similarly, the claim that dentistry suffers from an unjustified separation from other medical fields also has a great deal of truth to it, although this gap is slowly being closed.
However, using the example of one reckless practitioner to paint the whole profession, and to make misinformed claims about the lack of an evidential base for dentistry is completely unwarranted.
Given that the author identifies the public’s tendency to “belittle the medical significance [of dental procedures]”, as part of the problem, he must see the irresponsibility in adding to this by claiming (falsely) that dentistry lacks the empirical grounding of other medical disciplines.